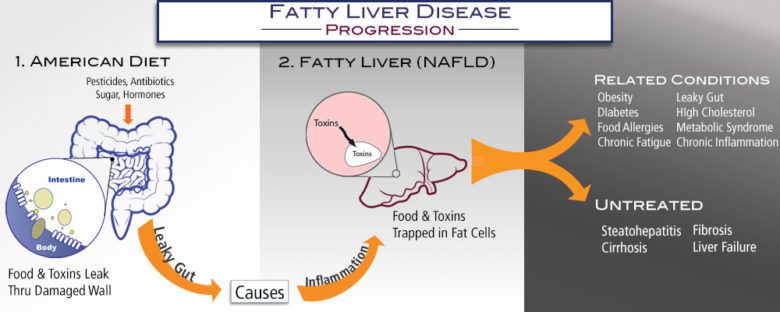
Non alcoholic Fatty Liver Disease (NAFLD) affects about one-third of Americans. That’s over 130 million people and most are completely unaware and go undiagnosed for years. In the beginning, there are typically no pain sensations, allowing it to progress silently. Symptoms of NAFLD range from diabetes, obesity, Irritable Bowel Syndrome ( IBS) to chronic fatigue, food allergies and metabolic syndrome. With the exception of obesity, all of these can come on with very few people even noticing.
Disease Progression
Left untreated NAFLD morphs into more advanced stages like non-alcoholic steatohepatitis, fibrosis, cirrhosis, and liver failure. Adults are not alone; shockingly 10% of children in America are also effected .1 Statistics for people living with advanced liver diseases are grim.
mechanism
NAFLD is the accumulation of fat cells in the liver, interrupting normal liver function in the absence of alcohol consumption. Although this kind of liver damage is common among alcohol consumers, this disease now effects those with diets high in processed foods with similar results. This typically causes inflammation and in more severe cases tissue death and fibrosis.
Excess fat cells accumulate in the liver beginning a destructive cycle and the liver becomes less efficient, leading to a build-up of toxins including fatty acids and insulin. The result is insulin resistance in type II diabetes. Tests that confirm the overload of fatty acids known as lipotoxicity can lead to metabolic syndrome and NAFLD.
In the past, the scientific community had been confused about the causes of NAFLD; now recent studies point to a leaking gut with an influx of free floating food particles and toxins in the body as a culprit. Leaky Gut is an improper balance of bacteria in the body leading to intestinal wall breach with a destructive cascade of health problems.
When the liver can no longer detoxify the influx of foreign substances they are swept into fat cells to be broken down later. While the obesity it produces can be observed externally, dangerous conditions compromise the health of the body’s organs internally.
There are two main systems designed to remove these invaders–the immune system and the liver. As Americans consume increasing amounts of sugar, caffeine, antibiotics, GMOs, pesticides, and hormones these two systems become overwhelmed. A further discussion on how the liver works including the two main phases is located here.
WHAT DOESN’T WORK
The pharmaceutical industry has been working on cures for NAFLD and related diseases with little success. Thus far Metformin has had the only successful attempt by the industry. Metformin has limited effectiveness as it is an insulin-sensitizing drug that only addresses part of the issue. Though it represents a marked improvement over preceding pharmaceutical alternatives.
WHAT WORKS
Fortunately, nature provides us with the solution. Studies demonstrate that Silybin (active compound in milk thistle), SAMe, NAC, Phosphatidylcholine and Glutathione work best with repeatable results. The success of these natural ingredients relies on rapid replenishment of Glutathione, a critically important liver antioxidant. 2, 3
Extracts from milk thistle have a long history in liver protection. Its rediscovery by science offers a renewed appreciation for its properties and health benefits. One very effective combination of silymarin, Vitamin E and Phosphatidylcholine, is an improvement in insulin sensitivity while reversing damaged liver cells reducing oxidative stress and improving Glutathione levels in the liver. 4, 5
All of these critical ingredients are found in HEPATIBEN.
We have done this in the pursuit to simplify solving this health issue.
N-acetyl cysteine (NAC) is a sulfur-rich compound used primarily to neutralize the damaging effects of aspirin on the liver. It rapidly restores Glutathione. A recent animal study finds it prevents NAFLD in a liver disease diet 6. Similarly, SAMe had been found to increase Glutathione levels in humans with Fatty Liver Disease. 7
Very few, if any products on the market contain all these ingredients and they are very expensive when purchased individually. To address this Liver Medic formulated Hepatiben to make fighting this battle easier, more effective and less expensive than the alternatives.
While we have discussed the mechanism and treatment for the liver, we can’t ignore the source of the problem. A healthy diet promotes a healthy gut and is critically important in ensuring that fatty liver disease does not return.
Often missed in efforts to restore healthy flora is the removal of biofilm, which is a frequent obstacle in improving gut health. Serrapeptase is nature’s most powerful weapon in this fight. Our enteric-coated Serrapeptase breaks apart biofilm to remove viruses, parasites and other harmful organisms. In combination with Candida Complex, is a great way to remove the bad actors and get healthy again.
available for purchase
References
- Polyzos SA, Kountouras J, Zavos C, Tsiaousi E. The role of adiponectin in the pathogenesis and treatment of nonalcoholic fatty liver disease. Diabetes Obes Metab. 2010 May;12(5):365-83.
- Kwon do Y, Jung YS, Kim SJ, Park HK, Park JH, Kim YC. Impaired sulfur-amino acid metabolism and oxidative stress in nonalcoholic fatty liver are alleviated by betaine supplementation in rats. J Nutr. 2009 Jan;139(1):63-8.
- Caballero F, Fernandez A, Matias N, et al. Specific contribution of methionine and choline in nutritional nonalcoholic steatohepatitis: impact on mitochondrial S-adenosyl-L-methionine and glutathione. J Biol Chem. 2010 Jun 11;285(24):18528-
- Loguercio C, Federico A, Trappoliere M, et al. The effect of a silybin-vitamin E-phospholipid complex on nonalcoholic fatty liver disease: a pilot study. Dig Dis Sci. 2007 Sep;52(9):2387-95.
- Serviddio G, Bellanti F, Giudetti AM, et al. A silybin-phospholipid complex prevents mitochondrial dysfunction in a rodent model of nonalcoholic steatohepatitis. J Pharmacol Exp Ther. 2010 Mar;332(3):922-32.
- Baumgardner JN, Shankar K, Hennings L, Albano E, Badger TM, Ronis MJ. N-acetylcysteine attenuates progression of liver pathology in a rat model of nonalcoholic steatohepatitis. J Nutr. 2008 Oct;138(10):1872-9.
- Vendemiale G, Altomare E, Trizio T, et al. Effects of ora oral S-adenosyl-L-methionine on hepatic glutathione in patients with liver disease. Scand J Gastroenterol. 1989 May;24(4):407-15.
additional articles

Which is the Best Liver Supplement for Fatty Liver?
Are you experiencing fatigue, abdominal discomfort, or unexplained weight gain? These could be signs of a fatty liver, a condition affecting millions worldwide. With lifestyles often characterized by poor dietary choices and sedentary habits, the prevalence of fatty liver disease

How Can I Detox my Liver in 7 Days?
Have you ever felt like your body needs a reset? Perhaps you are experiencing low energy levels, bloating, or just a general sense of malaise. If so, your liver might be trying to tell you something. Could a 7-day liver

What It Takes to Choose the Best Liver Cleanse Supplements?
In a world inundated with toxins and stressors, our liver, the unsung hero of detoxification, often bears the brunt. It’s no wonder many are turning to liver cleanse supplements to support this vital organ. But how do you navigate the
Supplements to Alleviate Fatty Liver Woes- Do You Concur?
Fatty liver, a prevalent health concern, often goes unnoticed until symptoms manifest. Addressing these symptoms and considering the incorporation of supplements can be pivotal in promoting liver health. But how effective are supplements for fatty liver, and what key nuances
Unlocking Liver Wellness: Choosing the Best Liver Detox Supplement
Detoxifying your liver is a crucial step towards maintaining overall health, especially in a world where environmental toxins and poor dietary choices are prevalent. But how do you embark on this journey, and is opting for a liver detox supplement

Nurturing Liver Health: Exploring Fatty Liver Medicine
Fatty liver, a prevalent health concern in the contemporary world, necessitates a strategic approach for long-term well-being. Let’s delve into the intricacies of fatty liver, understand the considerations for effective management,. It is crucial to explore the best possible scenarios